UNIT 4 - COOKING SESSION |
Dietary Management for Heart Disease
The role of diet in coronary heart disease is evident from its pathological process, which involves the formation of arterial plaques, alterations in endothelial function, heightened risk for thrombosis, and inflammatory processes. Diet plays a role through the regulation of blood lipids and by influencing endothelial function and the underlying inflammation that causes disease progression.
Diets promoting cardiovascular health should begin early because the atherosclerosis that contributes to coronary artery disease begins in childhood. A modified diet, particularly if combined with regular physical activity, can prevent, delay, or reverse the progression of atherosclerosis and development of coronary heart disease, with subsequent reduction in cardiovascular event.
Diets promoting cardiovascular health should begin early because the atherosclerosis that contributes to coronary artery disease begins in childhood. A modified diet, particularly if combined with regular physical activity, can prevent, delay, or reverse the progression of atherosclerosis and development of coronary heart disease, with subsequent reduction in cardiovascular event.
WORKING ON BLOOD LIPID LEVELS
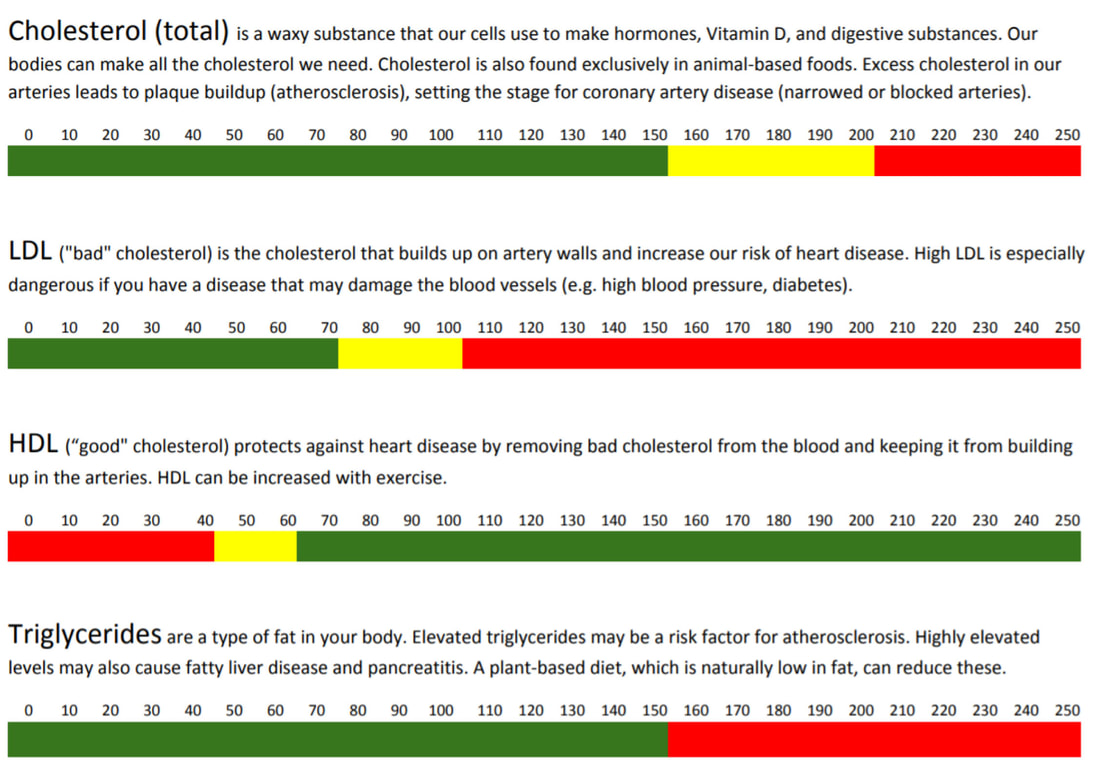
Saturated fats, trans fats, and cholesterol in the diet increase concentrations of blood lipids, particularly LDL cholesterol, while soluble fiber tends to reduce them. Controlling blood lipoprotein concentrations with a combination of diet, exercise, and medication, if necessary, is a cornerstone of treatment for most coronary heart disease patients.
Saturated fats, trans fats, and cholesterol in the diet increase concentrations of blood lipids, particularly LDL cholesterol, while soluble fiber tends to reduce them. Controlling blood lipoprotein concentrations with a combination of diet, exercise, and medication, if necessary, is a cornerstone of treatment for most coronary heart disease patients.
IMPROVING ANTIOXIDANT STATUS AND ENDOTHELIAL FUNCTION
Dietary antioxidants, folate, magnesium, and other substances in foods may reduce the burden of oxidized LDL and improve endothelial function through increased availability of nitric oxide. Endothelial dysfunction, represented by an increase in blood levels of asymmetric dimethylarginine (ADMA), is a strong predictor of coronary events and coronary mortality. ADMA increases after high-fat meals.
REDUCING INFLAMMATION
The role of inflammatory processes in atherosclerosis is increasingly apparent. Loss of excess body fat reduces C-reactive protein, an indicator of inflammation.
Decreasing dietary saturated fat and cholesterol.
Following diets low in saturated fat and cholesterol can help reduce progression of atherosclerosis. The National Cholesterol Education Program has recommended moderate reductions in total fat (< 30% of energy), saturated fat (< 7% of energy) and cholesterol (<200 mg/d) intake. In clinical trials such changes reduces plasma LDL cholesterol concentration about 5%.
Studies suggest that low-fat vegetarian and vegan regimens are significantly more effective, reducing LDL cholesterol approximately 15% to 13%. Because such regimens have also been shown to reduce body weight and blood pressure and to be useful in programs for reversing atherosclerosis, they may be preferable to many patients, provided they are prescribed along with basic diet instruction. combining daily aerobic exercise with a healthful diets adds to its benefits, particularly with regard to weight and blood glucose control.
Trans fatty acids, found in partially hydrogenated oils used in processed foods and margarines, increase LDL cholesterol and tend to reduce HDL cholesterol. Trans fatty acids also have pro-inflammatory effect similar to those of saturated fat and adversely affect vascular reactivity, reducing arterial flow-mediated dilation (a direct measure of vascular endothelial function) by 29% on diets containing 8% of calories from trans fat. The balance of dietary fats can be altered by the elimination of animal products, tropical oils the leading sources of saturated fats), and partially hydrogenated vegetable oils (trans fats).
Dietary antioxidants, folate, magnesium, and other substances in foods may reduce the burden of oxidized LDL and improve endothelial function through increased availability of nitric oxide. Endothelial dysfunction, represented by an increase in blood levels of asymmetric dimethylarginine (ADMA), is a strong predictor of coronary events and coronary mortality. ADMA increases after high-fat meals.
REDUCING INFLAMMATION
The role of inflammatory processes in atherosclerosis is increasingly apparent. Loss of excess body fat reduces C-reactive protein, an indicator of inflammation.
Decreasing dietary saturated fat and cholesterol.
Following diets low in saturated fat and cholesterol can help reduce progression of atherosclerosis. The National Cholesterol Education Program has recommended moderate reductions in total fat (< 30% of energy), saturated fat (< 7% of energy) and cholesterol (<200 mg/d) intake. In clinical trials such changes reduces plasma LDL cholesterol concentration about 5%.
Studies suggest that low-fat vegetarian and vegan regimens are significantly more effective, reducing LDL cholesterol approximately 15% to 13%. Because such regimens have also been shown to reduce body weight and blood pressure and to be useful in programs for reversing atherosclerosis, they may be preferable to many patients, provided they are prescribed along with basic diet instruction. combining daily aerobic exercise with a healthful diets adds to its benefits, particularly with regard to weight and blood glucose control.
Trans fatty acids, found in partially hydrogenated oils used in processed foods and margarines, increase LDL cholesterol and tend to reduce HDL cholesterol. Trans fatty acids also have pro-inflammatory effect similar to those of saturated fat and adversely affect vascular reactivity, reducing arterial flow-mediated dilation (a direct measure of vascular endothelial function) by 29% on diets containing 8% of calories from trans fat. The balance of dietary fats can be altered by the elimination of animal products, tropical oils the leading sources of saturated fats), and partially hydrogenated vegetable oils (trans fats).
Increasing dietary fiber
Soluble fiber, as is found in oats, barley, and beans, is particularly helpful in this regard. Sources of soluble dietary fiber and pectin, found mainly in fruits and vegetables, have also reduced atherosclerotic progression.
Consuming soy products
Both epidemiologic and clinical studies have shown that soy products (e.g. soymilk and meat substitutes) may reduce CHD risk. In addition to reducing blood lipids, soy has cardioprotective effects, such as lowering oxidized LDL, homocysteine, and blood pressure.
Clinical trials have combined these dietary lipid-lowering strategies. A vegetarian diet emphasizing cholesterol-lowering foods (including oats, soy foods, nuts, and plant sterols) appears to be particularly effective, lowering LDL cholesterol concentration approximately 30%, an effect similar to that of treatment with lovastatin.
Increasing fruits and vegetables
Fruits and vegetables can help reduce atherosclerosis and lower risk for coronary heard disease, particularly if the diet is low in saturated fat. However, the benefits of these foods go beyond their having no cholesterol, very little saturated fat, and abundant fiber. Among their active components are vitamin C, antioxidant flavonoids, and folic acid.
Soluble fiber, as is found in oats, barley, and beans, is particularly helpful in this regard. Sources of soluble dietary fiber and pectin, found mainly in fruits and vegetables, have also reduced atherosclerotic progression.
Consuming soy products
Both epidemiologic and clinical studies have shown that soy products (e.g. soymilk and meat substitutes) may reduce CHD risk. In addition to reducing blood lipids, soy has cardioprotective effects, such as lowering oxidized LDL, homocysteine, and blood pressure.
Clinical trials have combined these dietary lipid-lowering strategies. A vegetarian diet emphasizing cholesterol-lowering foods (including oats, soy foods, nuts, and plant sterols) appears to be particularly effective, lowering LDL cholesterol concentration approximately 30%, an effect similar to that of treatment with lovastatin.
Increasing fruits and vegetables
Fruits and vegetables can help reduce atherosclerosis and lower risk for coronary heard disease, particularly if the diet is low in saturated fat. However, the benefits of these foods go beyond their having no cholesterol, very little saturated fat, and abundant fiber. Among their active components are vitamin C, antioxidant flavonoids, and folic acid.
Food Preparation
You may access all the recipes listed below. Choose one recipe in each category and create 1 set of meal course that you can recommend to patients/clients or your family member. All recipes have instructions that you may also use as guide. Document your activity by taking photos of each recipe, starting from Mise en place up to the final presentation with brief description of your planned meal.
Unit Task
Please organize your documentation in a single file and send us the completed task using PDF format.